Facial Retraining – Neuromuscular
NEUROMUSCULAR RETRAINING FOR FACIAL PARALYSIS
“Rehabilitation can not be administered to the patient, in contrast to the treatment for many other disorders. The psychosocial and educational aspects of the rehabilitation process are thus of very great importance. In spite of the existence of biological bases for recovery, it does not occur without the appropriate environment, the attitude, and the involvement of the patient.”51
Neuromuscular retraining (NMR) for facial paralysis is a marriage of neurophysiology, psychology, therapeutic science, learning theory, and art. Neuromuscular retraining is a problem solving approach to treatment using selective motor training to facilitate symmetrical movement and control undesired gross motor activity (synkinesis). Tools such as surface EMG (sEMG) feedback and specific mirror exercises provide augmented sensory information to enhance neural adaptation and learning 38. The application of learning theory maximizes motivation through individualized instruction and active patient participation. Because each patient presents a different functional profile, there are no generic lists of exercises. Treatment is based on individual function, and as a result, each treatment program is different.
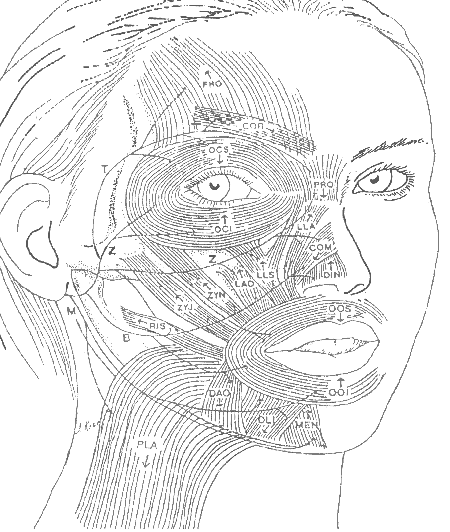
Patient education is the most basic aspect of the therapeutic process and lays the necessary foundation for learning the selective movement patterns that will improve motor function. The facial therapist provides training in basic facial anatomy, physiology and kinesiology pertinent to each patient’s specific situation. To familiarize them with muscle terminology and actions, patients receive the following graphic (Fig. 1) depicting the major facial muscle groups, branches of the facial nerve and the angles of muscular pull.
As each muscle group is evaluated the patient observes the action of that group in the mirror, bilaterally. Most people are not conscious of the specific movements involved in normal facial expression. To identify the correct response, patients are instructed to perform small, specific movements on the contralateral side . This exploration of facial movement is a time of discovery for the patient as s/he identifies the specific areas of function and dysfunction and begins to formulate strategies to improve facial movement .
| corrugator depressor labii inferioris levator labii superioris alaeque nasi orbicularis oris inferioris orbicularis oculi superioris risorius |
COR DLI LLA OOI OCS RIS |
depressor anguli oris frontalis levator labii superioris orbicularis oris superioris platysma zygomaticus major |
DAO FRO LLS OOS PLA ZYJ |
dilator naris levator anguli oris mentalis orbicularis oculi inferioris procerus zygomatiicus minor |
DIN LAO MEN OCI PRO ZYN |
Facial nerve branches: temporal (T), zygomaticus (Z), buccal (B), mandibular (M) and cervical (C)
General Treatment Principles
Treatment is based on the functional profile rather than etiology. Techniques to facilitate movement and inhibit abnormal patterns refine motor control, coordination and complexity of movement. Although each patient’s program differs, there are common aspects of the treatment of all patients.
Slow Execution
Initiating movements slowly and gradually allows the patient to observe and modify the angle, strength, and speed of the excursion as it occurs.52 As a result, new motor control strategies are systematically developed and learned.39 Movements performed rapidly will revert to the previous, abnormal motor pattern.
Small Movements
Small movements preserve isolated responses of the facial muscles by limiting motor unit recruitment to those muscles targeted.39 Large movements recruit successively greater numbers of motor units as well as neighboring muscles (overflow), diminishing accuracy39. Improved coordination develops as small movements are practiced accurately.
Symmetry
Patients are instructed in symmetrical excursion of movements to reinforce the normal physiological response. Attempts to produce symmetrical movements initially include limiting excursion on the contralateral side. If the contralateral side is allowed to dominate, activity on the involved side could be diminished.46
Action-oriented and Cost-Effective Therapy
Just as no surgical technique provides the patient with normal, synchronous facial movement, neuromuscular retraining cannot restore perfect function. However, these action-oriented techniques enable patients to “become their own best therapist”53, and assume control of their recovery resulting in improved physical function, increased self-esteem and satisfaction.54
Treatment schedules are based on individual patient needs which vary widely. Factors such as motivation, compliance, need for sEMG feedback, and geographic location affects scheduling. Treatment sessions may range from 2 hours per month (for local patients) to an intensive treatment session of 9-12 hours spaced over 3-4 days, every 6 months (for patients traveling a great distance). This differs significantly from a typical therapy schedule in which patients are treated on a weekly basis. A limited schedule can be maintained in a neuromuscular retraining program because the therapist provides educational rather than “hands-on” treatment and the patient directly controls the practice of his or her own therapy program at home.
A patient may be involved in neuromuscular retraining for three years or longer. It has been estimated that the average ratio of home practice to supervised clinical instruction is about 20:1.38. Structuring therapy in this manner results in a cost-effective service delivery system that reduces the number of billed clinic hours while increasing the overall number of treatment hours. Patients return to the clinic periodically to refine movement patterns, learn new exercises, document progress and establish new treatment goals.