Facial Retraining – Specific Techniques
SPECIFIC TECHNIQUES FOR TREATING FLACCID PARALYSIS AND SYNKINESIS
Clinically, facial paralysis falls into two categories:
– Flaccid paralysis (complete facial paralysis) or paresis
– Synkinesis or mass action (varying degrees of motor weakness accompanied by abnormal, unsynchronous facial movements).
The two types of paralysis require different treatment strategies.
Flaccid Paralysis/Paresis
The therapist determines the presence of activity using clinical evaluation methods and sEMG. Slight movement that is undetectable by the patient or physician is made visible by sEMG feedback which reinforces the proper movement pattern and illustrates the presence of muscle activity to the patient. Retraining strategies begin with slow, small, symmetrical movements which are continued during home program practice. The patient should be followed monthly to record changes, modify the home program and monitor for the development of synkinesis. Detailed protocols for the treatment of flaccid paralysis, including sEMG training, have been outlined elsewhere.68,70
Decreased facial sensation, often associated with facial paralysis, limits awareness of the affected side and may hinder the ability to learn new motor behaviors.74 Sensory re-education techniques can be applied to enhance awareness.68,74
Synkinesis/Mass Action
The primary feature of the treatment of synkinesis is inhibition of the unwanted, aberrant movements that occur with volitional and spontaneous movements. Abnormal, synkinetic movement may have the effect of working antagonistically, like a “tug-of-war”, against the normal, primary movement. For example, a patient who demonstrates zygomatic activity trying to smile, but also has synkinesis of the platysma, has limited zygomatic excursion. Instead of the characteristic upward curl at the angle of the mouth (a smile), s/he has a drawing down at the angle of the mouth (a grimace). By inhibiting the synkinesis of the platysma, the zygomatic gains a more normal range of motion without the antagonistic effect of the platysma. The result is a more natural smile.
Any of the facial muscle groups can be involved in synkinesis to varying degrees. The challenge is to identify the sites of synkinesis and teach the patient effective inhibition techniques. As inhibition of synkinesis takes place, the range of the primary movement gradually extends, increasing excursion, strength, and isolated motor control simultaneously.
Reduce Resting Tone
Increased facial tone, tightness or rigidity may be noted in any area of the affected face and is most likely caused by increased background muscle activity.59 Signs may include increased nasolabial fold (levators, zygomaticus), decreased palpebral fissure (orbicularis oculi), retraction of the corner of the mouth (zygomaticus, risorius), dimpling of the chin (mentalis and/or depressors) drawing down of the corner of the mouth (depressors and platysma), and banding of the neck (platysma). Abnormal tone of the lips may present as thinning or “puffiness”.
Because normal movement can not be superimposed on abnormal tone,39,75 the first stage of neuromuscular retraining for the patient with synkinesis is to decrease hypertonus. Therapists begin by making patients aware that facial stiffness or tightness is caused by increased muscle activity at rest. General relaxation training and sEMG feedback47,68 are effective tone reduction techniques.
Massage mobilizes the tissues of the affected side where thickening and immobility are observed.76,77 Using the opposite thumb on the inside of the cheek and the 2 and 3 digit on the facial skin, patients are taught to draw the tissues toward the mouth. Patients will often encounter a trigger point, an area of discrete pain caused by focal contraction of that motor unit, which will resolve with maintained deep pressure.78 Patients report increased comfort and mobility after several weeks of practice.
Inhibition of Synkinesis
With attention focused on the precise movement pattern, the patient initiates the primary movement slowly, monitoring the area of synkinesis from the start. As synkinesis becomes visible, the primary movement is maintained while the synkinetic response is reduced. This difficult process requires complete concentration in order to “release” the synkinetic area. Once this is achieved, the patient then relaxes the primary movement. The exact timing of this sequence is essential for dissociation of synkinesis from primary movement.
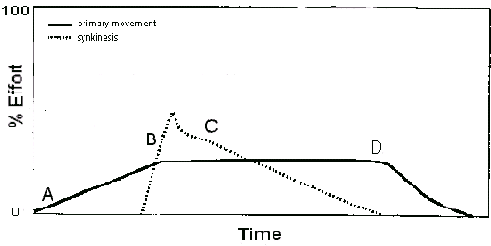
As the patient becomes proficient in performing the exercise, inhibition of synkinesis requires less concentration, and excursion of the primary movement increases as control is learned. Initially, this movement pattern can only be accomplished volitionally, however, in time, these patterns are demonstrated spontaneously.47,68Figure 3: Recommended strategy for inhibition of synkinesis. The Patient initiates the primary movement (A) while monitoring area of synkinesis. As synkinesis becomes apparent (B), the patient maintains activity of the primary mover while releasing the synkinesis (C). After the synkinesis is inhibited, the patient relaxes the primary movement (D). The duration of this process is typically 10 to 20 seconds.
Botulinum Toxin (Botox) Injection for Reducing Synkinesis
Botulinum toxin injections have been found to reduce aberrant contractions of the facial muscles by blocking the acetylcholine receptor sites at the synapse.48,79,80 Botox temporarily paralyzes targeted areas of synkinesis, (usually orbicularis oculi inferioris, platysma and mentalis) with effects lasting 4 to 6 months.79 When combined with neuromuscular retraining, Botox provides a “window of opportunity” during which the patient can practice more normal movement patterns without synkinetic interference. In some cases, patients experience decreased synkinesis after the injection effects have worn off.81
XII-VII anastomosis
Neuromuscular retraining for the patient with a hypoglossal (XII) anastomosis is similar to treatment of synkinesis. However, the motor nucleus of the XIIth cranial nerve must learn to control the facial musculature. Two additional steps to the ones described for synkinesis are required to improve motor control:
Step 1 – The patient allows movement of the tongue to initiate facial movement, but only until s/he begins to make minimal movements of the face without activating the tongue.
Step 2 – The patient learns to inhibit facial movement while the tongue moves. This step reduces the aberrant facial movement seen during speech and mastication.
These difficult procedures require intense concentration. As the patient becomes adept at performing these movement patterns, s/he can begin to dissociate tongue from facial movements. These techniques are also effective with spinal accessory-facial nerve (XI-VII) anastomosis, substituting shoulder movement for tongue movement.
DURATION AND PROGRESSION OF TREATMENT AND FOLLOW-UP
The entire course of neuromuscular retraining typically lasts from 12 months to 3 years. Exercises are progressed as successive short-term goals are attained during this relatively slow process. Long-term goals may take years to achieve, therefore it is unrealistic to expect this process to occur quickly.38
Videotape and photographic reevaluations are completed approximately every six months or as significant functional change is noted. Patients actively participate in comparing the initial to subsequent evaluations, identifying new problem areas and establishing new goals.
REFERRAL TO OTHER MEDICAL SPECIALISTS
During the course of neuromuscular retraining, it may be necessary to refer patients to other healthcare providers. Prolonged lack of eye closure and lacrimation may lead to ophthalmologic referral for gold weight, spring placement or other procedure. Plastic surgeons may be consulted for nerve grafting, muscle transposition or related procedures. In cases of severe depression, psychology or psychiatry referrals may be indicated. Rehabilitation specialists may be able to assist patients with vestibular problems. Audiologists can provide hearing assistive devices. Timely referrals to appropriate health care providers are essential in providing optimal care for the facial paralysis patient.